Serving Cleveland, Lyndhurst & Westlake, OH
Serving Cleveland, Lyndhurst & Westlake, OH
Surgical treatment for migraine headache
(peripheral trigger point decompression)
Meet our Migraine Surgeon Dr. Totonchi
Dr. Totonchi is Professor of Plastic Surgery at Case Western Reserve University in Cleveland, Ohio, He is based at MetroHealth Hospital which is part of the plastic Surgery Division, and serves as medical director of craniofacial anomalies clinic. He also serves the east and west side of the town in more private office settings. He has been involved with migraine surgery treatment and research for a long time and since has been discovered and presented by Dr. Bahman Guyuron. Dr. Totonchi has been fortunate to be part of his team at multiple levels like postdoctoral research fellow, graduated from his residency program working closely with this group of patients, and did a clinical fellowship with him.
Dr. Totonchi has also been involved with research in this field and has multiple publications on this topic. He has also been one of the faculty members of the annual course for surgical treatment of migraine headaches from 2006 to this year, lecturing, serving in the panels, and teaching national and international attendees in the course and cadaver lab.
Migraine Headache
 Migraine is a complex neurological disorder in which genetics is a prominent underlying factor. Headache is the most common presenting symptom of migraine and can sometimes be a debilitating condition. Migraine runs in about 18 million Americans, it is 3 times more common in females than males, Management of migraine should always start with pharmacological(medication) and/or non-pharmacological (diet, exercise…) approaches by patients’ primary care physician or neurologists, complicated cases will need a referral to neurologists specialized in headache or experienced in dealing patient with migraine headache.
Migraine is a complex neurological disorder in which genetics is a prominent underlying factor. Headache is the most common presenting symptom of migraine and can sometimes be a debilitating condition. Migraine runs in about 18 million Americans, it is 3 times more common in females than males, Management of migraine should always start with pharmacological(medication) and/or non-pharmacological (diet, exercise…) approaches by patients’ primary care physician or neurologists, complicated cases will need a referral to neurologists specialized in headache or experienced in dealing patient with migraine headache.
A small percentage of patients who do not respond adequately to medications or have side effects to the medications are considered for migraine surgery.
Who is a candidate for surgery?
All of the patients should be seen and evaluated by a neurologist, preferably a Headache specialist to rule out other reasons for the headache, and also to make sure that all available treatments are tried adequately. Patients who do not respond to medical treatments or have side effects are potential candidates for surgery.
We prefer for the patients who are on chronic narcotic use or barbiturate use( like Fioricet) to be detoxified before surgery. Detoxification from these medications certainly will decrease the headache frequency and intensity and this simple process may even eliminate the need for surgery altogether.
The other group of patients are the ones who do not have severe migraine headaches or their headaches are responding to medication but are considering a cosmetic procedure, these groups of patients should notify us before cosmetic surgery since migraine surgery could be a very minor addition to their cosmetic surgery.
What is Migraine surgery?
Migraine surgery is based on trigger point release. Currently, there are 4 main trigger points, the release of these trigger points can improve or eliminate migraine headaches. Although not every migraine sufferer has all of them but a combination of active trigger points are very common, there are also some less common trigger points that have been described as well.
Main Migraine Trigger Points: (click on links to learn more)
- Frontal trigger point
 Surgery can be done with minimally invasive techniques (endoscopically) using few 1 cm hairline incisions or by direct upper eyelid incision. This surgery usually takes about 1-2h based on the technique used.
Surgery can be done with minimally invasive techniques (endoscopically) using few 1 cm hairline incisions or by direct upper eyelid incision. This surgery usually takes about 1-2h based on the technique used.
- Temporal trigger point
 Surgery can be done with minimally invasive techniques (endoscopically) which is our preferred technique, some direct approach through line hairline incision or upper eyelid incision have been described. Migraine surgery usually takes about 30min-1h.
Surgery can be done with minimally invasive techniques (endoscopically) which is our preferred technique, some direct approach through line hairline incision or upper eyelid incision have been described. Migraine surgery usually takes about 30min-1h.
- Nasal trigger point
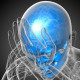 Surgery can be done endoscopically, by direct vision or combination. This surgery usually takes about 30min-1h based on the technique used and severity of the pathology.
Surgery can be done endoscopically, by direct vision or combination. This surgery usually takes about 30min-1h based on the technique used and severity of the pathology.
- Occipital trigger point
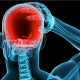 Migraine surgery for this site is done by an incision in the back of the scalp in the lower part of the hairline.
Migraine surgery for this site is done by an incision in the back of the scalp in the lower part of the hairline.
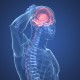
- Less common trigger points:
-
- Auriculotemporal trigger point: is located in the temporal area along the hairline, slightly outside of the usual temporal trigger point. The nerve can be irritated by the temporal artery or fascial band, surgery for this trigger point can be done in-office under local anesthesia using a small incision in 15-30 minutes.
-
- Lesser Occipital nerve: is located in the back of the head few centimeters outside of the greater Occipital nerve, surgery for this trigger point can be done in office or in operating room along with other trigger points.
- Peripheral trigger points: in some patients terminal branches of the the nerves mentioned before can be irritated by a blood vessel or a soft tissue band, this can be treated by a simple procedure in office.
-
In most of these trigger points there is a nerve which is compressed mostly by a muscle, artery, fascia, deviated septum or other intranasal pathology and triggering the patient’s migraine headache.
There is debate and controversy weather these headache should be called migraine headache or not, but all of the original articles published in this field by Dr. Guyuron seen by a neurologist and diagnosed with migraine based on International Classification of Headache Disorder classification.
Surgery is based on eliminating the pressure off the nerve and the technique to do this varies based on trigger point anatomy and functional considerations.
Migraine Surgery Frequently Asked Questions
Which trigger point surgery is right for me?
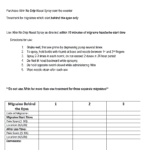
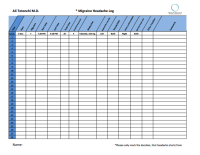
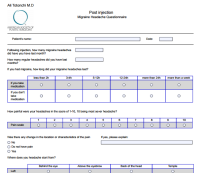
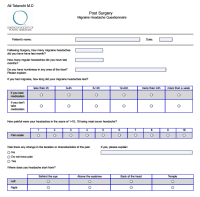
Determination of active trigger points is done during an office visit after evaluation of the patient’s CT scan (if indicated) along with studying the patient’s headache log and forms. Therefore it is very important for the patients to take their time to go over the forms and fill them out precisely. It is also important to note where the headache starts from rather than where it radiates to. Usually, patients remember the radiating part better than the starting point since pain stays in the radiated part for a longer time. In general:
- In patients with frontal trigger point, the headache starts from the eyebrow or above it, these patients may have strong frowning muscles. These patients often see an ophthalmologist before referring to a neurologist because they think their headache is due to some eye problems.
- In patients with temporal trigger points, headache usually starts in the temple area, These patients sometimes have a history of teeth grinding, clenching, and some of these patients diagnosed with a TMJ problem.
- Patients with nasal trigger point have pain behind the eye, and/or sinus area. These patients’ headaches are triggered by weather or barometric pressure change, they also might have some issues with breathing through the nose. These groups of the patients are often wrongly diagnosed with “sinus headache” and they usually are seen by Ear, Nose, Throat doctors, or allergist for years before they see headache specialists.
- In patients with occipital trigger point pain usually starts in the occipital area or back of the neck or shoulder. The headache usually starts in the afternoon and often we can find a tender point in the occipital area. These group of patients often seeks relief from chiropractic care and some of them have undergone unnecessary neck manipulation which could make the headache worse or cause other complications.
Although the above information is a kind of oversimplification of the symptoms, they are key points in identification of the trigger points.
What to expect after surgery?
All of these surgeries are done on an outpatient basis. Patients usually go home a couple of hours after surgery unless there is comorbidity or other medical issues which necessitate their hospital stay. Most of the time more than one trigger point is involved in a patient, and the postoperative course depends on how many trigger points have been operated on. as mentioned before the majority of the patient go home on the day of surgery they might have a small drain that usually will come out in 2-3 days after surgery. Pain: a patient might have a migraine headache the night of surgery which usually improves soon, surgical pain lasts a few days sometimes longer, patients will be given pain medications for surgical pain. final results usually are evaluated 3-6 months after surgery. At any time that patient notices pain reduction, they need to be seen by their neurologist to decrease or adjust migraine medications.
- Frontal and temporal trigger point surgery patients might have some swelling and bruising around the eyes for few days, I usually do not use the drain for this group of patient but I might be necessary in some group of patients. temporary numbness in the forehead usually happens and decreased over the time.
- Nasal trigger point: patients usually have nasal stent 7 to 10 days after surgery, the humidified room will help with their postoperative congestion
- Occipital trigger point: these patients usually are discharged home with the drain and it is usually removed 3-4 days after surgery
What are the complications of the surgery?
Infection and bleeding are very rare, local pain and severe itching may happen which improves over the time, scaring and very minor hair loss around the incision have been reported, occasionally patients have improved headache but they still experience aura or other migraine-related symptoms.
Should I continue taking my regular migraine medications?
Migraine medications need to be managed by a neurologist specialized or experienced in headache medicine, if you do not have a neurologist it is better to contact one who is familiar with the migraine surgery to see if you are a good candidate for surgery.
Neurologists working with our practice:
Cleveland/Akron Area:
Dr. Hossein Ansari
Dr. Ansari is Assistant professor of Internal medicine at NorthEast Ohio Medical University.
He finished his Neurology residency at West Virginia University followed by a fellowship in Headache Medicine at Mayo Clinic in Rochester, MN. Dr. Ansari is Board certified by the American Board of Psychiatry and Neurology and board-certified in Headache medicine by the united council of Neurological subspecialties. He is an active member of the American Academy of Neurology, American headache society, and International Headache Society and has had multiple presentations at national and international conferences. Dr. Ansari is currently director of the Headache center at Neurology and Neuroscience Associates in Akron, OH. appointments can be made by calling: (330) 572-1011 Ext 140 or visiting the website.
website: http://www.nnadoc.com/html/h_ansari.html
MetroHealth Hospital:
The neurology department in MetroHealth hospital offers a wide variety of services including headache treatment. Website: http://www.metrohealth.org/neurology
appointments can be made by calling: 800-554-5251 or visiting their website.
What is the success rate?
In properly selected patients, studies have shown that 80-90% of the patients have a positive response to surgery, defined by complete elimination or at least 50% reduction in headache severity or duration.
Is this surgery covered by Insurance?
Insurance coverage differs from company to company or coverage policy, which can be checked before the date of surgery. We also offer a self-pay package for the patient whom insurance companies do not cover the procedure.
Out of town patients:
We recommend for our out of town patients to stay in the area for 4-5 days so the wound can be monitored, a consultation can be done over the phone, and examination is usually done 1-2 days before surgery. Please click on the forms below to view and download them.